Exercise is important to improve strength, endurance, prevent health problems, reduce stress, and increase your energy levels. Symptoms such as fatigue, pain, breathlessness may make exercise difficult during this time. You may notice that your usual level of exercise, or even small amounts of activity have become difficult to manage. It is important to be aware that returning too quickly to intense exercise can worsen Long COVID symptoms. A gradual increase in exercise is important to safely manage your symptoms and prevent injury or exhaustion. If you are experiencing muscle or joint pains, feeling low in energy, or feel that your symptoms worsen after activity, try slowly increasing your exercise according to the five phases below.
Remember to stay on each phase for at least 7 days, and only move to the next phase if you do not feel fatigued or that your symptoms have increased. Drop back a phase if you experience setbacks in your symptoms.
Caution: If you feel chest pain, dizziness, lightheaded, or nausea, stop exercising and contact your healthcare provider. See your GP for a referral to a physiotherapist if you have ongoing concerns about exercise.
Phase 1 - gentle exercise that you can complete with ease.
This phase focusses on preparing you for a return to exercise.
Example exercises: Try practising breathing techniques, take a gentle walk, perform stretches, or balance exercises. You may do stretches while sitting or standing. Hold each stretch for 15-20 seconds.
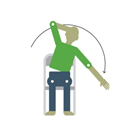 |
Reach your right arm up to the ceiling and then lean over to the left slightly; you should feel a stretch along the right side of your body. Repeat on the other side. |
 |
Put your arm out in front of you. Keeping your arm straight, bring it across your body at shoulder height, using your other hand to squeeze your arm to your chest so you feel a stretch around your shoulder. Repeat on the opposite side. |
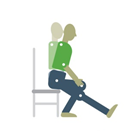 |
Sit on the edge of a chair with your leg out straight in front of you with your heel resting on the ground. Place your hands on your other thigh as support. Sitting as tall as you can, bend slightly forward at your hips until you can feel a slight stretch down the back of the leg that is stretched out. Repeat on the opposite side. |
 |
Stand with your feet apart, lean forward onto a wall and step one leg behind you. Bend your front knee, keeping your back leg straight and your heel on the floor. You should feel a stretch in the back of your lower leg. Repeat on the opposite side. |
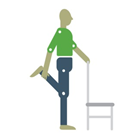 |
Stand up and hold onto something sturdy for support. Bend one leg up behind you, using the hand on the same side to hold your ankle or the back of your leg. Take your foot up towards your bottom until you feel a stretch along the front of your thigh. Repeat on the opposite side. |
Phase 2 - low intensity exercises
You should not face any breathing difficulties while doing Phase 2 exercises.
Example exercises include walking, doing light household or outdoor gardening tasks. If you can do these activities while holding a conversation with someone, you can increase the time you spend doing these activities by 10-15 minutes each day.
Phase 3 - moderate intensity exercises
Exercises in phase 3 may make you breathe heavily, but you should be able to have a conversation with someone while doing them.
Example exercises are brisk walking, climbing up and down stairs, jogging, introducing slopes or inclines to your walks, and performing resistance exercise.
Phase 4 - moderate intensity exercises which also train your coordination and functioning skills
Example exercises are running, cycling, swimming, and dance classes.
Phase 5 - baseline exercises
At this phase you should be able to do the types of exercise and activities that you could do before you got COVID-19.



 Long COVID doesn’t just affect people physically it can also affect other parts of a person’s wellbeing such as their mental health. To manage long COVID you need to take care of the different aspects of your life that support good wellbeing. The Māori model of health te whare tapa whā developed by Sir Mason Durie in 1984 uses the wharenui (meeting house) and its four walls to symbolise the different dimensions of health that contribute to wellbeing. The connection with the whenua (land) forms the foundation for 4 dimensions. The wharenui is strengthened by its four walls and secure foundation. Similarly, we are at our strongest when each dimension of our health is cared for. When any of the dimensions are challenged, we can draw strength from our foundation or another dimension to balance and strengthen our overall wellbeing. You may want to consider these different dimensions in relation to taking care of yourself during Long COVID.
Long COVID doesn’t just affect people physically it can also affect other parts of a person’s wellbeing such as their mental health. To manage long COVID you need to take care of the different aspects of your life that support good wellbeing. The Māori model of health te whare tapa whā developed by Sir Mason Durie in 1984 uses the wharenui (meeting house) and its four walls to symbolise the different dimensions of health that contribute to wellbeing. The connection with the whenua (land) forms the foundation for 4 dimensions. The wharenui is strengthened by its four walls and secure foundation. Similarly, we are at our strongest when each dimension of our health is cared for. When any of the dimensions are challenged, we can draw strength from our foundation or another dimension to balance and strengthen our overall wellbeing. You may want to consider these different dimensions in relation to taking care of yourself during Long COVID.
 If you are not sure how to talk to others about Long COVID, you can
If you are not sure how to talk to others about Long COVID, you can 
 Practising gratitude can improve your physical, psychological, social, and spiritual wellbeing. By feeling grateful we can improve our mood, sleep better, take better care of our bodies and minds, and improve our relationships with others.
Practising gratitude can improve your physical, psychological, social, and spiritual wellbeing. By feeling grateful we can improve our mood, sleep better, take better care of our bodies and minds, and improve our relationships with others. 





 Brain fog, which you might hear referred to as ‘cognitive dysfunction’, is a commonly reported symptom of Long COVID. People describe their thinking being slowed down, having trouble remembering things, having difficulty concentrating or focusing on tasks, having trouble tolerating loud noises, and finding it hard to find the words to say things. These symptoms can have a big impact on usual daily activities such as work or study as well as the ability to socialise.
Brain fog, which you might hear referred to as ‘cognitive dysfunction’, is a commonly reported symptom of Long COVID. People describe their thinking being slowed down, having trouble remembering things, having difficulty concentrating or focusing on tasks, having trouble tolerating loud noises, and finding it hard to find the words to say things. These symptoms can have a big impact on usual daily activities such as work or study as well as the ability to socialise.
 1. Plan
1. Plan 2. Prioritise
2. Prioritise Delegating or planning your tasks can help you save energy. Examples include doing your cooking in the weekend to prepare for the week ahead or grocery shopping online. Importantly, you do not have to go through long COVID alone. Reach out to your friends and whānau and let them help with challenging tasks such as shopping, preparing meals, or driving if they can.
Delegating or planning your tasks can help you save energy. Examples include doing your cooking in the weekend to prepare for the week ahead or grocery shopping online. Importantly, you do not have to go through long COVID alone. Reach out to your friends and whānau and let them help with challenging tasks such as shopping, preparing meals, or driving if they can.




















